However, there was still stretch-like pain in the right lower back, but it was tolerable.Ĭonclusions: For patients with polyostotic fibrous dysplasia combined with proximal femoral shepherd deformity and pathological fracture of the femoral shaft with nonunion, osteotomy combined with intramedullary nailing is a simple and convenient way to correct the deformity and obtain correct fracture alignment. One year after the operation, the patient could walk without a walker and take care of himself at home. After six months of re-examination, the patient could walk with a walker. The patient was instructed to gradually bear weight. It was found that the fractured end had a tendency to heal. Three months after the operation, he came to the hospital for re-examination, and an X-ray of the right femur was taken.
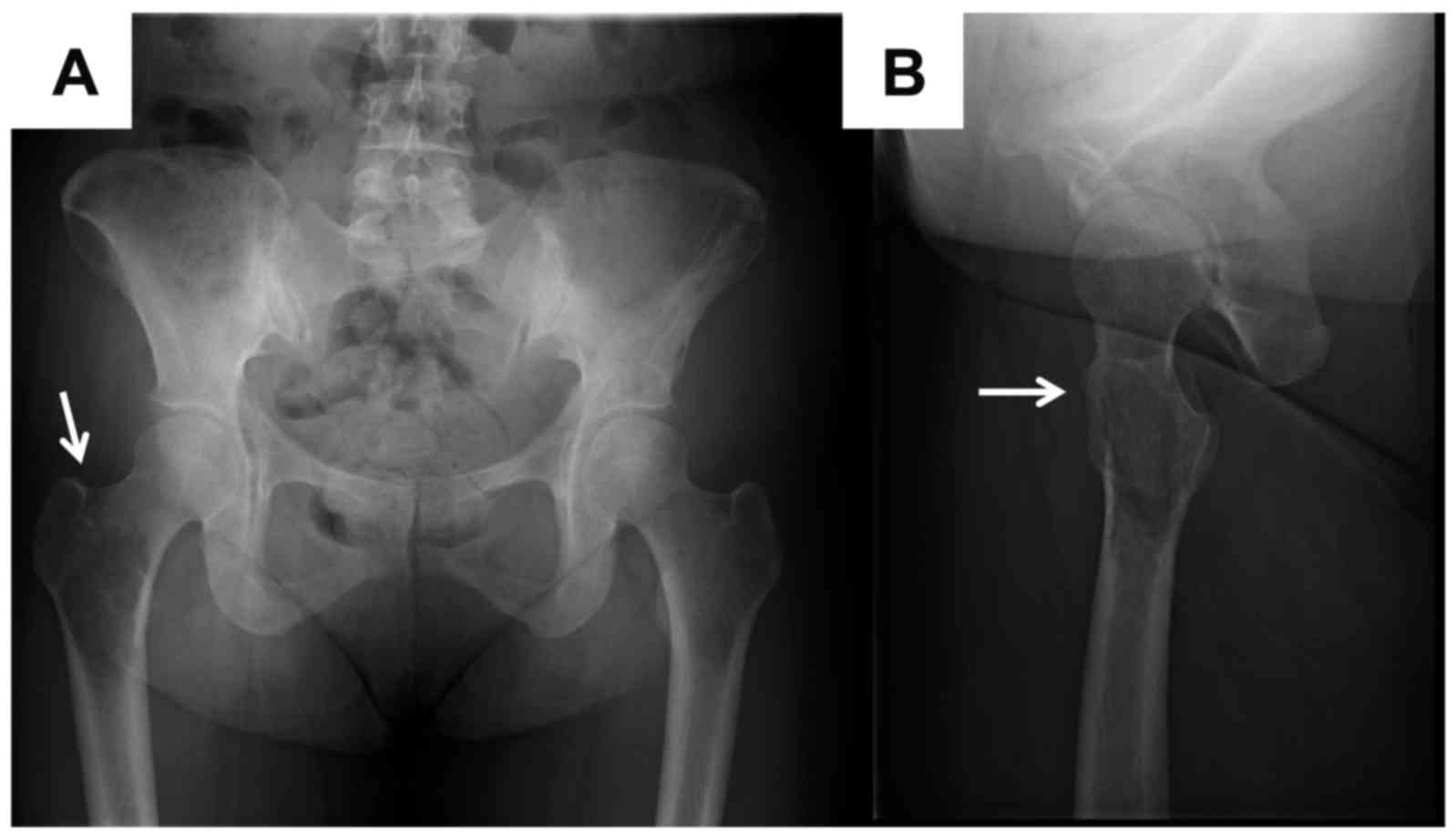
It is necessary to understand the disease in more detail to avoid overtreatment of benign lesions or misdiagnosis of malignant tumors and other diseases.Ĭase presentation: A 58-year-old man with polyostotic fibrous dysplasia, bilateral proximal femur deformity, Shepherd’s angle deformity, right femoral shaft pathological fracture complicated by nonunion, we under fluoroscopy, in the obvious proximal fracture, take osteotomy, and process the shape of the cut bone fragment to adapt it to the corrected force line, and then restore it back to its original position, using intramedullary nailing technology complete the operation. We report a patient with a rare case of multiple fibrous dysplasia combined with proximal femoral shepherd deformity with pathological fracture of the femoral shaft complicated by nonunion. It can manifest as simple fibrous dysplasia (70%–80%), polyostotic fibrous dysplasia (20%–30%), with approximately the same incidence in men and women. Introduction: Fibrous dysplasia is a benign fibrous bone tumor that accounts for 5% to 10% of benign bone tumors. 2The First Clinical Medical College of Bin Zhou Medical College, Binzhou, China.1Department of Orthopedics, The First Hospital of Jilin University, Changchun, China.Practical pointsĪccurate reporting of malignant vertebral fracture is important, as the diagnosis may affect the disease staging and treatment as well as the patient's prognosis.Qifan Yang 1, Jing Liu 2, Lei Tan 1, Ye Jiang 1 and Dong Zhu 1* convex bulging (not retropulsion) of the posterior vertebral cortex into the spinal canalĬontrast enhancement of the fractured vertebral body was in some studies 1 not helpful in differentiating between osteoporotic and metastatic vertebral fractures, as they both usually present with heterogeneous, intense enhancement.replaced signal of the vertebral body, especially extending into the pedicles or posterior elements (on MR).It is sometimes hard to differentiate between malignant and acute osteoporotic vertebral fractures, especially in elderly patients with known malignancy, as both types of fracture are prevalent in this population.įeatures that favor pathological fractures are: Radiographic features Pathological vs osteoporotic fractures

If there is a spinal cord or nerve root compression, respective neurologic deficits occur. As with other types of vertebral fractures, they present with pain and loss of mobility.
